Polycystic Ovary Syndrome (PCOS) is one of the most common hormonal disorders affecting women today. While it is often discussed in relation to fertility and married life, the truth is that PCOS can affect women at any stage—including unmarried women and even teenagers.
Unfortunately, many young women ignore early symptoms, assuming they are “normal hormonal changes.” This delay can worsen the condition over time.
In this detailed guide, we’ll explore the symptoms of PCOS in unmarried women, why they occur, and when you should take action.
What is PCOS?
PCOS (Polycystic Ovary Syndrome) is a hormonal imbalance where the ovaries produce higher-than-normal levels of androgens (male hormones).
This leads to:
- Irregular menstrual cycles
- Formation of small cysts in ovaries
- Metabolic and hormonal issues
Important: You don’t need to be married or sexually active to have PCOS.
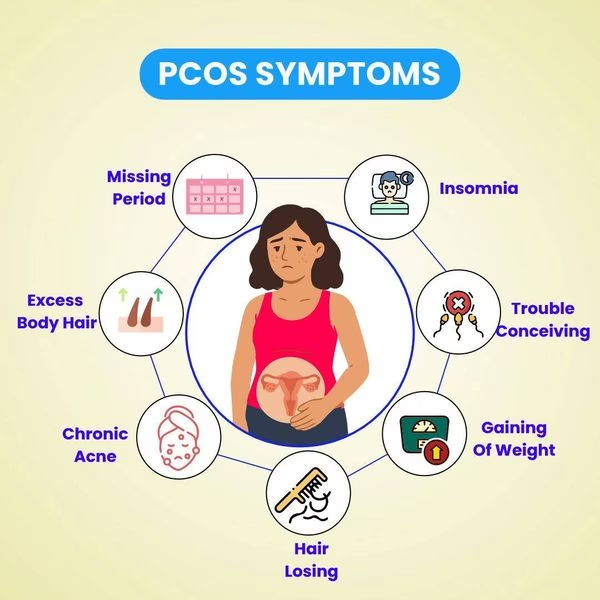
Common PCOS Symptoms in Unmarried Women
Here are the most common signs you should watch for:
1. Irregular Periods
One of the earliest and most noticeable symptoms.
You may experience:
- Delayed periods (cycles longer than 35 days)
- Missed periods for months
- Very light or very heavy bleeding
Why it happens: Hormonal imbalance affects ovulation.
2. Excess Hair Growth (Hirsutism)
Unwanted hair growth in areas like:
- Face (chin, upper lip)
- Chest
- Back
- Abdomen
This happens due to increased androgen levels.
3. Severe Acne and Oily Skin
If you’re dealing with persistent acne even after teenage years, it could be PCOS.
Common signs:
- Acne on jawline and chin
- Oily skin
- Breakouts that don’t respond to normal treatments
4. Sudden Weight Gain
Many women with PCOS struggle with:
- Rapid weight gain
- Difficulty losing weight
Especially around the abdomen.
5. Hair Thinning or Hair Fall
PCOS can cause:
- Hair thinning on scalp
- Male-pattern baldness in severe cases
6. Dark Patches on Skin (Acanthosis Nigricans)
You may notice dark, velvety skin in areas like:
- Neck
- Underarms
- Groin
This is linked to insulin resistance.
7. Mood Swings and Anxiety
Hormonal imbalance can affect mental health.
You may feel:
- Anxiety
- Depression
- Mood swings
8. Fatigue and Low Energy
Even after proper rest, you may feel:
- Constant tiredness
- Low motivation
9. Sugar Cravings and Insulin Resistance
PCOS often leads to insulin resistance.
Signs include:
- Frequent sugar cravings
- Feeling hungry often
- Energy crashes
10. Difficulty Losing Weight
Even with diet and exercise, weight loss becomes difficult due to hormonal imbalance.
Causes of PCOS in Unmarried Women
While the exact cause is unknown, common factors include:
- Genetics (family history)
- Insulin resistance
- Hormonal imbalance
- Lifestyle factors (diet, stress, lack of exercise)
When Should You See a Doctor?
You should consult a doctor if you notice:
- Irregular or missed periods
- Excessive hair growth
- Persistent acne
- Sudden weight gain
Early diagnosis helps prevent complications.
Can PCOS Be Managed?
Yes, PCOS is manageable with the right approach.
1. Healthy Diet
Focus on:
- Low glycemic foods
- High fiber
- Protein-rich meals
Avoid:
- Sugary foods
- Processed snacks
2. Regular Exercise
- 30 minutes daily activity
- Cardio + strength training
3. Stress Management
- Yoga
- Meditation
- Deep breathing
4. Medical Treatment
Doctors may prescribe:
- Hormonal pills
- Insulin-sensitizing drugs
Myths About PCOS in Unmarried Women
❌ Myth 1: Only married women get PCOS
👉 Truth: PCOS can affect anyone after puberty
❌ Myth 2: PCOS only affects fertility
👉 Truth: It affects overall health
❌ Myth 3: You must have cysts to have PCOS
👉 Truth: Not always
Final Thoughts
PCOS is not just a condition for married women—it’s a lifestyle and hormonal disorder that can begin early in life.
Recognizing the symptoms early can help you:
- Manage the condition effectively
- Prevent long-term complications
- Improve overall quality of life
If you notice multiple symptoms, don’t ignore them. Early action makes a huge difference.
FAQs
-
Can unmarried women have PCOS?
Yes, PCOS can affect women regardless of marital status.
-
What is the first sign of PCOS?
Irregular periods are usually the first sign.
-
Is PCOS curable?
PCOS is not completely curable but can be managed effectively.
-
Does PCOS affect future fertility?
It can, but early management improves chances.
-
Can PCOS go away on its own?
No, but symptoms can improve with lifestyle changes.