Polycystic Ovary Syndrome, commonly known as PCOS, is one of the most prevalent hormonal disorders affecting women of reproductive age. It impacts various aspects of health, from menstruation to fertility, and can cause long-term complications if not addressed properly.
Understanding the symptoms, causes, and treatment options of PCOS is crucial for managing this condition and improving quality of life.
What Is PCOS?
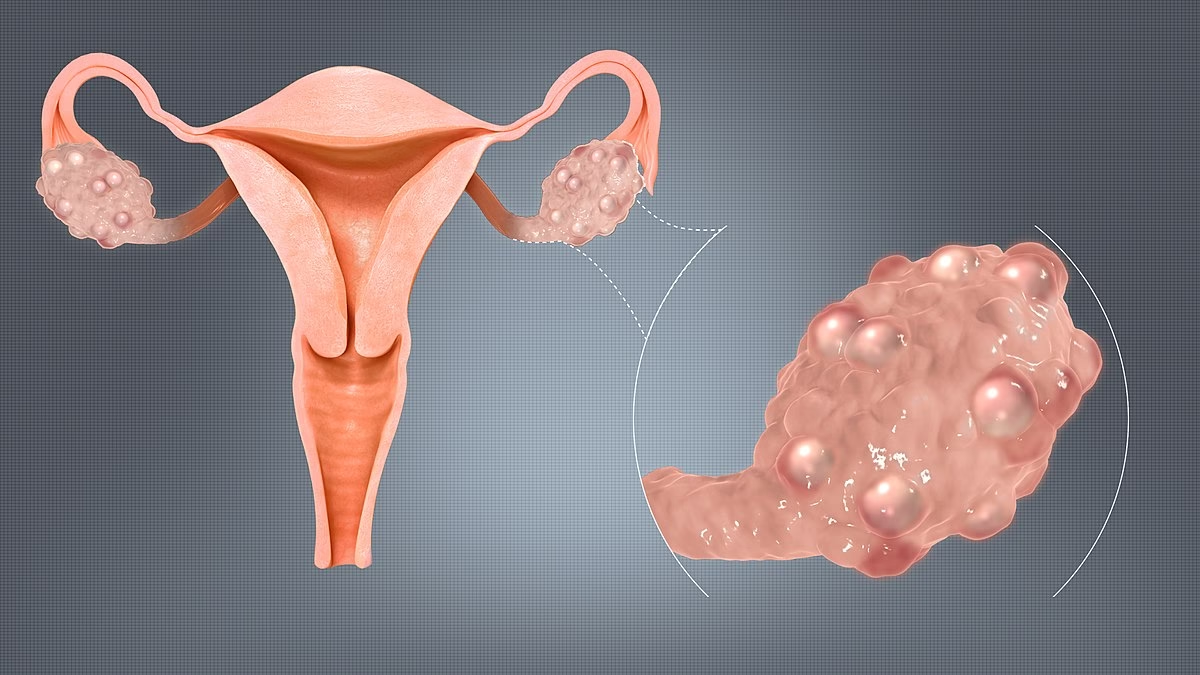
PCOS (Polycystic Ovary Syndrome) is a hormonal disorder that occurs when a woman’s ovaries produce an abnormal amount of androgens (male hormones). This imbalance disrupts ovulation and can lead to multiple small cysts in the ovaries, irregular menstrual cycles, and other health issues. This condition nowadays affect teenage girls too. PCOS symptoms like hormonal imbalance in teenage girls are get confused with “normal puberty changes”
Note: It is different but often confused with PCOD (Polycystic Ovary Disease). PCOS typically refers to a hormonal imbalance, while PCOD refers to a structural issue in the ovaries.
Common Symptoms of PCOS
Women suffering from PCOS may experience a variety of symptoms, which vary in intensity:
- Irregular or absent menstrual cycles
- Difficulty getting pregnant (polycystic ovaries pregnancy challenges)
- Excessive hair growth on face, chest, or back (hirsutism)
- Acne and oily skin
- Weight gain, especially around the abdomen
- Thinning hair or hair loss
- Darkening of skin in body folds
- Fatigue and mood swings
Recognizing these early can help in early diagnosis and treatment.
What Causes PCOS?
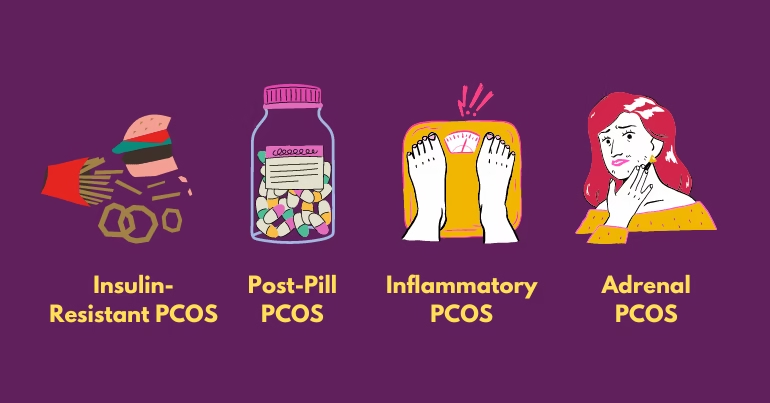
The exact reason of PCOD or PCOS remains unclear, but several factors are believed to contribute:
Hormonal Imbalance
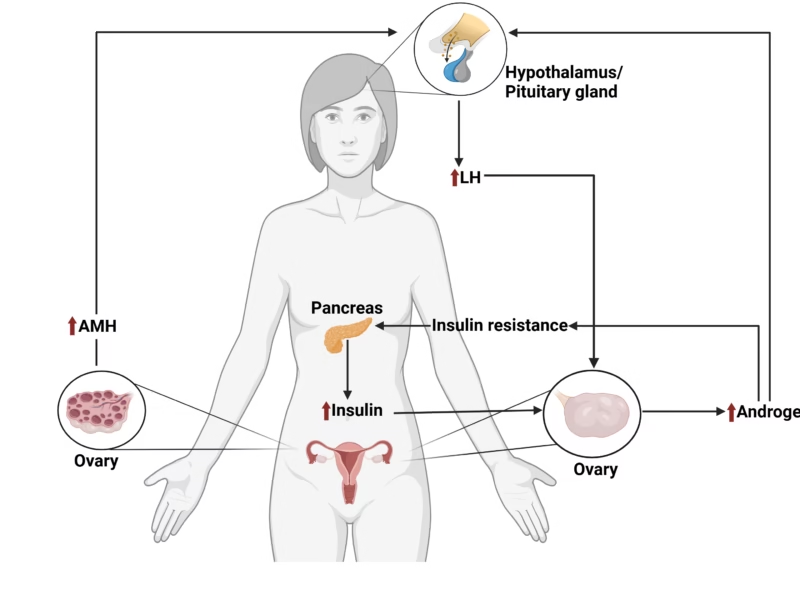
An increase in male hormones (androgens) interferes with ovary function, preventing regular ovulation.
Insulin Resistance
High insulin levels can cause the ovaries to produce more androgens. Many women with PCOS are overweight or obese, which worsens insulin resistance.
Genetic Factors
Family history plays a role. If your mother or sister has polycystic overies, your risk is higher.
Low-Grade Inflammation
Chronic low-level inflammation may trigger androgen production by the ovaries.
The cause is often multifactorial, combining genetics, lifestyle, and environmental factors.
Effects of PCOS on Health
PCOS is more than a reproductive disorder. The effects of PCOS can be widespread:
- Infertility due to lack of ovulation
- Increased risk of developing type 2 diabetes
- Higher chance of cardiovascular disease
- Obesity
- Sleep apnea
- Mental health issues (depression, anxiety)
- Endometrial cancer due to prolonged lack of periods
Early diagnosis and a healthy lifestyle are key to managing long-term risks.
How PCOS Is Diagnosed
Diagnosing PCOS involves a combination of symptom evaluation, medical history, and specific tests. There is no single test for PCOS, so doctors use a set of criteria and investigations to confirm the condition.
Rotterdam Criteria (2 out of 3 Rule)
Doctors commonly use the Rotterdam criteria to diagnose PCOS. A diagnosis is made if at least two of the following three features are present:
- Irregular or absent ovulation, which may show up as irregular periods
- Signs of excess androgens, such as acne, hair thinning, or excess facial and body hair
- Polycystic ovaries visible on ultrasound
Blood Tests
Blood tests are done to check hormone levels and rule out other conditions. These may include:
- Androgen levels (testosterone)
- Luteinizing hormone (LH) and follicle-stimulating hormone (FSH)
- Thyroid function tests
- Prolactin levels
- Blood sugar and insulin levels
Ultrasound Scan
A pelvic ultrasound helps examine the ovaries and uterus. In PCOS, the ovaries may appear enlarged and contain multiple small follicles. However, not everyone with PCOS will have visible cysts, and having cysts alone does not confirm PCOS.
Conditions to Rule Out
Since PCOS shares symptoms with other health conditions, doctors may rule out:
- Thyroid disorders
- Hyperprolactinemia
- Adrenal disorders
- Cushing’s syndrome
A proper diagnosis is important because it helps guide the right treatment plan and ensures that other underlying conditions are not missed.
Treatment Options for PCOS
Although there’s no permanent cure, many treatments can help manage the symptoms:
Lifestyle Changes
- Balanced diet focused on whole foods
- Regular physical activity
- Weight management helps improve insulin sensitivity and hormone balance.
Medications
- Hormonal birth control pills: Regulate menstrual cycles and reduce androgen levels.
- Metformin: Helps improve insulin sensitivity and may regulate periods.
- Clomiphene Citrate: Used to stimulate ovulation for those trying to get pregnant.
- Anti-androgens (like spironolactone): Help reduce excess hair growth and acne.
Natural Remedies
- Spearmint tea, inositol supplements, and cinnamon have shown promise in reducing androgen levels and improving insulin resistance.
Long-Term Health Risks of PCOS
PCOS is not just a short-term hormonal condition. If left unmanaged, it can increase the risk of several long-term health complications. Being aware of these risks can help you take early steps to protect your overall health.
Type 2 diabetes
Insulin resistance is very common in PCOS, which can lead to consistently high blood sugar levels over time. This significantly increases the risk of developing type 2 diabetes, especially if lifestyle factors are not managed.
Heart disease
PCOS is linked to risk factors such as high cholesterol, high blood pressure, and obesity. These can contribute to cardiovascular problems, increasing the likelihood of heart disease in the long run.
Infertility
Hormonal imbalances can interfere with regular ovulation, making it more difficult to conceive. While many people with PCOS can still get pregnant with the right support, untreated PCOS can lead to ongoing fertility challenges.
Endometrial issues
Irregular or absent periods can cause the uterine lining (endometrium) to build up over time. This may increase the risk of endometrial hyperplasia and, in some cases, endometrial cancer if not properly managed.
Mental health concerns
PCOS can have a significant impact on emotional well-being. Many individuals experience anxiety, depression, mood swings, and low self-esteem due to hormonal changes and physical symptoms.
Understanding these risks highlights the importance of early diagnosis and consistent management to reduce complications and support long-term health.
Polycystic Ovaries and Pregnancy
Having polycystic ovaries pregnancy is possible but can be more challenging due to irregular ovulation or hormonal imbalance. Many women with PCOS still conceive naturally or with the help of fertility treatments. Early diagnosis and treatment improve the chances of a healthy pregnancy.
Tip: Always consult a gynecologist or fertility specialist for personalized care.
Can You Get Pregnant with PCOS?
Yes, you can get pregnant with PCOS. While it may take more time or support, many people with PCOS go on to have healthy pregnancies. The key is understanding what might be affecting fertility and choosing the right approach to manage it.
Ovulation Issues
PCOS often affects ovulation due to hormonal imbalances. The ovaries may not release an egg regularly, which can lead to irregular or missed periods. Without consistent ovulation, it becomes harder to predict fertile windows and conceive naturally. However, ovulation is not always completely absent—it may just be irregular, which means pregnancy is still possible.
Treatment Options
There are several ways to improve fertility with PCOS, depending on individual needs.
- Lifestyle changes such as maintaining a healthy weight, balanced diet, and regular exercise can help regulate ovulation
- Medications may be prescribed to stimulate ovulation or improve insulin sensitivity
- In some cases, fertility treatments like assisted reproductive techniques may be recommended
The right treatment plan can significantly increase the chances of conception.
A Hopeful Perspective
PCOS is one of the most common and treatable causes of infertility. With proper guidance, many people are able to regulate their cycles and conceive successfully. Even small, consistent changes in lifestyle can make a meaningful difference over time.
If you are trying to conceive, you are not alone—and with the right support, pregnancy is absolutely possible.
Final Thoughts
Polycystic Ovary Syndrome (PCOS) affects many women globally, but it doesn’t have to dictate your life.
✅ Recognize the symptoms early
✅ Understand the pcod reason and contributing factors
✅ Take action through lifestyle changes, medical treatments, and natural remedies
Managing PCOS is about long-term health and not just temporary fixes. Empower yourself with knowledge and take small steps toward a balanced life.
Your health is your greatest asset. 🌸